HISTORY
Hepatotoxicity dates back to nearly 100 years. Just recently, they have discovered that some of the most common drugs can cause liver injury. These drugs are currently well known to the public and used by a majority of the population. The drugs in question are known as non-steroid anti-inflammatory drugs (NSAIDS), statins, anti-diabetics, and acetaminophen.
- Acetaminophen was known to cause liver damage in 1943, if not taken in therapeutic range. Even when taken appropriately, can cause hepatotoxicity if taken with other medications.
- The anti-diabetic drug, troglitazone, was the first drug to bring light to hepatotoxicity and the long-term causes it can have on the liver.
TODAY
Hundreds of articles exist on the effects of drugs on the liver. The drug industry has been hit hard with removal of drugs from the market that cause liver damage. Liver hepatotoxicity is one of the most common reasons that drugs are withdrawn from the public's use. Even doses in the therapeutic range, have been known to cause toxicity of the liver. Although these drugs were known to work effectively, they were shown to cause severe liver damage, liver transplant, or death.
In 2006, the FDA added guidelines to follow if the immune system falls below a certain range. Liver enzymes should be tested in order to keep patients safe. This is currently the only way to diagnosis liver hepatoxicity, at least the most efficient way.
Recently, the public has become aware of acetaminophen related hepatotoxicity. One controversy on OTC drugs is the drug-drug interactions. The public is not as educated as they should be on the ease of overdosing on OTC drugs. As healthcare professionals, it should be an important goal to educate patients on liver safety.
WHAT THE FUTURE HOLDS
Drug companies will have a never-ending battle with regulating the side effects of drugs. It could be considered a catch 22, drugs can dramatically improve ones life and at the same time be a silent killer. The FDA has taken steps to educate the public on these drugs, but the warnings do not seem to be eye catching enough.
Studies show that there is a possible genetic link to drug induced liver injury. Science Daily (2009) studies show that acetaminophen is toxic if taken in high doses, but a link exists showing that toxicity is more likely due to genetics. The study suggests that finding the genetic marker will help create safer drugs in the future. Studies also suggest that some patients become more susceptible due to their environmental factors.
Current preclinical and clinical liver safety testing does an excellent job in keeping the public safe from drugs capable of causing various forms of liver injury.
In any case, the FDA will constantly be on alert for drugs and their contraindications for hepatotoxicity. Healthcare professionals will need to be aware of the ever-changing revisions to drugs and safety changes.
References:
Lucena, M., García-Cortés, M., Cueto, R., Lopez-Duran, J., & Andrade, R. (2008). Assessment of drug-induced liver injury in clinical practice. Fundamental & Clinical Pharmacology, 22(2), 141-158. http://search.ebscohost.com/
Watkins, P. (2005). Idiosyncratic liver injury: challenges and approaches. Toxicologic Pathology, 33(1), 1-5. http://search.ebscohost.com/
Fontana R, Watkins P, Bonkovsky H, et al. Drug-Induced Liver Injury Network (DILIN) prospective study: rationale, design and conduct. Drug Safety: An International Journal Of Medical Toxicology And Drug Experience [serial online]. 2009;32(1):55-68. Available from: MEDLINE
Ipswich, MA. Accessed October 16, 2009.Lee W, Senior J. Recognizing drug-induced liver injury: current problems, possible solutions. Toxicologic Pathology [serial online]. 2005;33(1):155-164. Available from: MEDLINE, Ipswich, MA. Accessed October 16, 2009.009.




I work at TGI Fridays and in our TABC program we are told that it takes about one drink per hour to leave the system. When i serve guests sometimes they will order three and sometimes even four during there visit, I will be thinking twice next time i serve my guests. Also, when i serve i dont think about the combination of both alcohol and acetaminophen, i will now though. Is it harmful to combine acetaminophen with other things, like medicines?
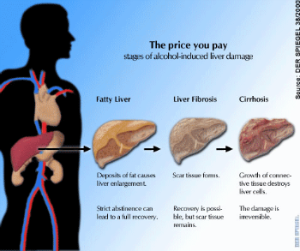
ReplyDeleteI have lost people close to me due to Alcoholic Cirrohosis. It is a sad sight. Hopefully my liver will repair itself after all of my years of drinking and the damage done to my liver.
ReplyDeleteHi Steven,
ReplyDeleteYes, it can be harmful when combining acetaminophen with other medications! Cholesterol lowering drugs, antibiotics, and antidiabetics are just a few of the drugs that can also harm your liver! Think about those in combination with alcohol!! Even 2 drinks might be have serious consequences for your liver!! What do you think about taking Tylenol for "hangovers"?
Hello Anonymous,
Alcoholism is very devastating. Changing your lifestyle is difficult but essential to your health. The liver is amazing at repairing itself, but complications from long term exposure to toxins can arise. Here are some websites to check out specific to your situation:
http://www.liverfoundation.org/education/info/alcohol/
http://www.hepatitis.va.gov/vahep?page=basics-13-00
I really dont think people who drink bother to think about all the damage that could be done to all aspects of their life and health.
ReplyDeleteSome people just don't know the damage that can be done when drinking. The average person drinks, at least moderately. The key here is getting the word out so that people who do drink, even if only socially, realize the dangers associated with alcohol. More often than not, the same person may be taking a drug that can react with alcohol in the liver, such as Tylenol. Is it an inability to comprehend what they are doing to themselves, a lack of knowledge, or the cycle of addiction that makes people seem careless? It all depends...
ReplyDeleteI found this information very helpful! I knew not to mix alcohol with medicine, but I did not know that consumption could cause many different diseases. I will most definitely educate people when I see then drinking way too much!
ReplyDeleteEmily,
ReplyDeleteI think that it's great that you want to continue the message on to others! That is the only way most people would ever find out about the risks associated with alcohol.